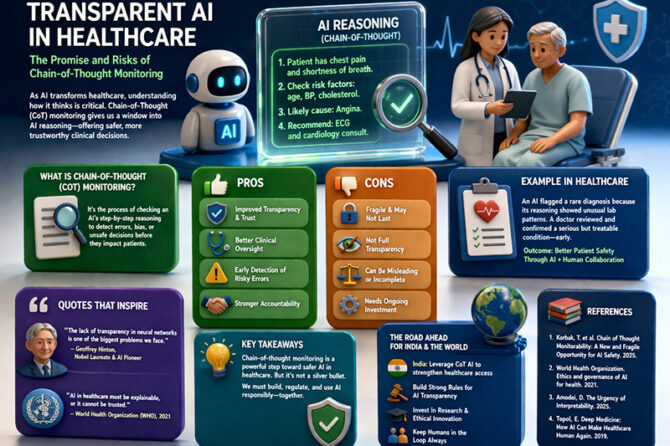
The greatest risk associated with artificial intelligence in the healthcare sector today is not the slow adoption of the technology; it is the rapid adoption of the technology, which is far outstripping the development of the governance structures that can support it in a safe, equitable, and accountable manner. This issue has been repeatedly highlighted in the global policy discourse. The World Health Organization, in its guidelines on AI ethics in 2021, cautioned that the rapid adoption of AI in the healthcare sector can lead to an escalation of harm, bias, and inequity in the already vulnerable healthcare system. Within this context, the Strategy for Artificial Intelligence in Healthcare (SAHI), which was released by the Ministry of Health and Family Welfare in the country, is an effort that is timely and pragmatic.
SAHI is grounded in the expansion of the digital public infrastructure in the country, including the Ayushman Bharat Digital Mission that seeks to create interoperable health records and standardized data exchange systems. Unlike the regulatory environment that can be overly restrictive in its approach and can stifle innovation in the sector, the SAHI is grounded in a risk-based approach. This is in line with the international best practices in AI governance in the healthcare sector that have been recommended by organizations such as the Organisation for Economic Co-operation and Development, which recommends the development of “trustworthy AI” that is grounded in transparency, accountability, and human values (OECD AI Principles, 2019). While not all AI applications in the healthcare sector pose the same level of risk, SAHI enables the rapid scaling up of low-risk AI applications such as administrative support or appointment systems.
This philosophical underpinning of SAHI, which posits the role of AI in augmenting human judgment rather than replacing it, resonates with the assertion of the medical practitioner and author Eric Topol in his book “Deep Medicine”published in 2019: “AI has the potential to restore the human side of medicine rather than detract from it.” This means that the role of AI systems in the health sector must be seen as one of assistance and not of replacement. For example, the role of AI in improving the detection of early-stage cancers via radiology systems must be seen in the context of verification by human experts. Research published in the journal “Nature Medicine” has demonstrated the benefits of collaboration between human experts and AI systems in achieving better results compared to the application of either approach in isolation. This collaboration has been demonstrated in studies published in the journal “Nature Medicine” in which the collaboration of human experts and AI systems was seen to be more successful compared to the application of either approach in isolation (Esteva et al., 2019).
However, the success of such collaboration depends on the presence of certain foundational elements. The success of AI systems in the health sector depends more on the integration of such systems in the real world rather than the performance of the systems in the laboratory. The quality of the data remains one of the challenges in the application of AI systems in the health sector. The presence of fragmented data has been seen to affect the reliability of the results obtained from the application of AI systems. The presence of racial bias in the application of AI systems in the health sector has been demonstrated in the landmark review published in the journal “Science” in which Obermeyer et al. demonstrated the presence of racial bias in the application of AI systems in the health sector. The presence of heterogeneous IT systems in low- and middle-income countries remains one of the challenges in the application of AI systems in the health sector.
From an Indian point of view, tremendous opportunities exist. AI has the potential to alleviate workforce shortages, expand diagnostics to rural areas, and improve efficiencies in high-volume public sector institutions. For instance, AI-based screening tools have been piloted in India to detect diabetic retinopathy. On the other hand, the potential harms are equally considerable. If not properly managed, AI-based tools have the potential to perpetuate errors, undermine accountability, and compromise patient trust. As noted by NITI Aayog in their national AI strategy (2018), “the challenge is not just to adopt AI, but to adopt it responsibly.”
Similar tensions can also be seen at the international level. The European Commission has proposed an AI Act, which classifies healthcare AI as “high risk” and proposes stringent compliance. Although it is positive from a safety point of view, it has also been argued that over-regulation can act as an inhibitor to innovation. The Indian SAHI, on the other hand, attempts to find a middle ground between flexibility and principle, and adaptability and accountability. The future of AI in healthcare, therefore, depends as much on technological advancements as it does on the maturation of healthcare systems. As Topol aptly puts it, “technology alone is not the solution; it is how we use it that matters.” In this regard, perhaps the most significant contribution of SAHI is to shift the debate from adoption to integration.
Dr. Prahlada N.B
MBBS (JJMMC), MS (PGIMER, Chandigarh).
MBA in Healthcare & Hospital Management (BITS, Pilani),
Postgraduate Certificate in Technology Leadership and Innovation (MIT, USA)
Executive Programme in Strategic Management (IIM, Lucknow)
Senior Management Programme in Healthcare Management (IIM, Kozhikode)
Advanced Certificate in AI for Digital Health and Imaging Program (IISc, Bengaluru).
Senior Professor and former Head,
Department of ENT-Head & Neck Surgery, Skull Base Surgery, Cochlear Implant Surgery.
Basaveshwara Medical College & Hospital, Chitradurga, Karnataka, India.
My Vision: I don’t want to be a genius. I want to be a person with a bundle of experience.
My Mission: Help others achieve their life’s objectives in my presence or absence!
My Values: Creating value for others.
References:
- World Health Organization. Ethics and governance of artificial intelligence for health. Geneva: WHO; 2021.
- Eric Topol. Deep Medicine: How Artificial Intelligence Can Make Healthcare Human Again. New York: Basic Books; 2019.
- Esteva A, Robicquet A, Ramsundar B, Kuleshov V, DePristo M, Chou K, et al. A guide to deep learning in healthcare. Nature Medicine. 2019;25(1):24–29.
- Obermeyer Z, Powers B, Vogeli C, Mullainathan S. Dissecting racial bias in an algorithm used to manage the health of populations. Science. 2019;366(6464):447–453.
- Organisation for Economic Co-operation and Development. OECD Principles on Artificial Intelligence. Paris: OECD; 2019.
- NITI Aayog. National Strategy for Artificial Intelligence #AIforAll. New Delhi: Government of India; 2018.
- European Commission. Proposal for a Regulation laying down harmonised rules on Artificial Intelligence (Artificial Intelligence Act). Brussels: European Union; 2021.
- Ministry of Health and Family Welfare. Strategy for Artificial Intelligence in Healthcare (SAHI). Government of India; (latest available policy document).
















Dear Dr. Prahlada N. B Sir,
Your insightful blog post on AI in healthcare resonates deeply with the current landscape. The Strategy for Artificial Intelligence in Healthcare (SAHI) is a commendable initiative, emphasizing a risk-based approach to ensure safe and equitable adoption 🌟.
Key highlights from your post:
– *Governance over Speed*: Rapid AI adoption risks outweigh benefits without robust governance structures.
– *Human-AI Collaboration*: AI should augment human judgment, not replace it, as seen in cancer detection via radiology.
– *Challenges Ahead*: Data quality, racial bias, and heterogeneous IT systems hinder AI integration.
SAHI's focus on digital public infrastructure and interoperability is crucial for India's healthcare transformation. The collaboration between Karnataka and the Netherlands showcases promising advancements in AI-driven healthtech.
Looking forward to exploring more on AI's role in enhancing healthcare accessibility and outcomes. 🙏
Reply